华南理工大学学报(自然科学版) ›› 2025, Vol. 53 ›› Issue (10): 155-173.doi: 10.12141/j.issn.1000-565X.240258
盐酸安非他酮对SD大鼠肠道菌群耐药组的影响
闫鹤1, 陈春霞1, 刘宗保2, 李佳林1, 詹诗皿1
- 1.华南理工大学 食品科学与工程学院/广东省天然产物绿色加工与产品安全重点实验室,广东 广州 510640
2.广西师范大学 生命科学学院,广西 桂林 541006
-
收稿日期:2024-05-27出版日期:2025-10-25发布日期:2024-11-29 -
作者简介:闫鹤(1972—),女,博士,副研究员,主要从事食品微生物研究。E-mail: yanhe@scut.edu.cn -
基金资助:国家自然科学基金项目(32170064)
Effects of Bupropion Hydrochloride on Resistome of Gut Microbiota in SD Rats
YAN He1, CHEN Chunxia1, LIU Zongbao2, LI Jialin1, ZHAN Shimin1
- 1.School of Food Science and Engineering/ Guangdong Provincial Key Laboratory for Green Processing of Natural Products and Product Safety,South China University of Technology,Guangzhou 510640,Guangdong,China
2.College of Life Sciences,Guangxi Normal University,Guilin 541006,Guangxi,China
-
Received:2024-05-27Online:2025-10-25Published:2024-11-29 -
About author:闫鹤(1972—),女,博士,副研究员,主要从事食品微生物研究。E-mail: yanhe@scut.edu.cn -
Supported by:the National Natural Science Foundation of China(32170064)
摘要:
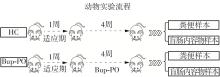
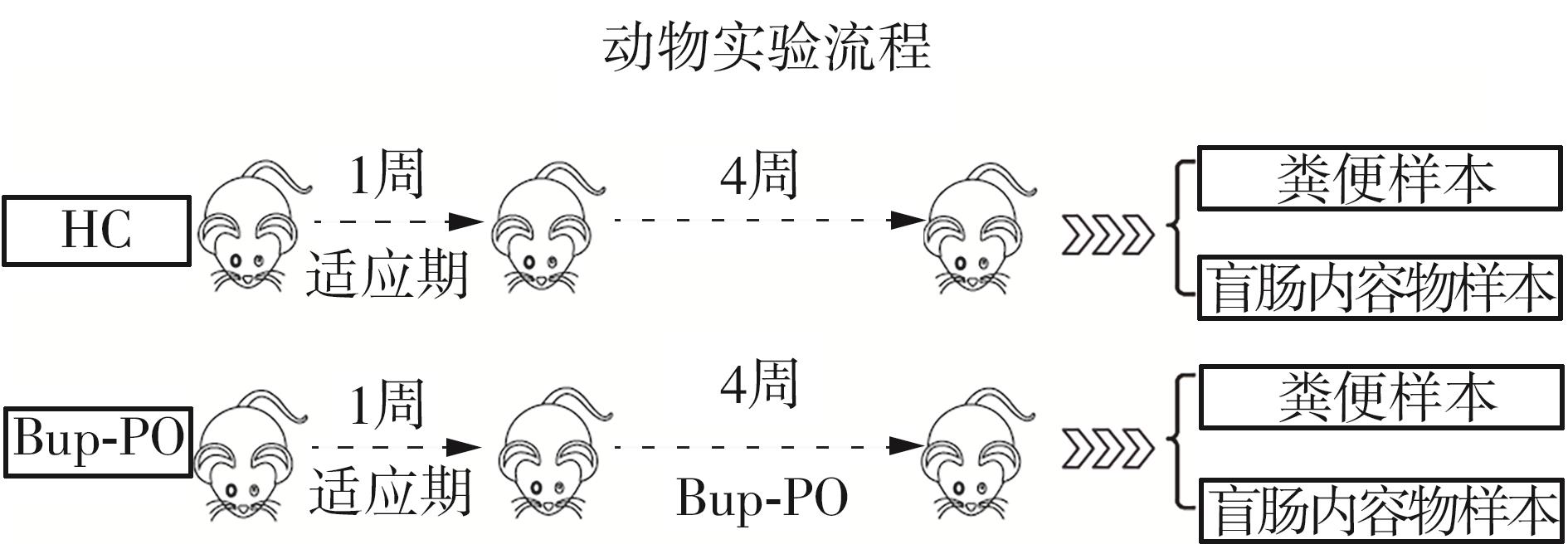
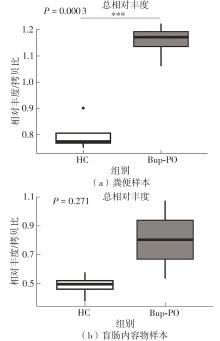
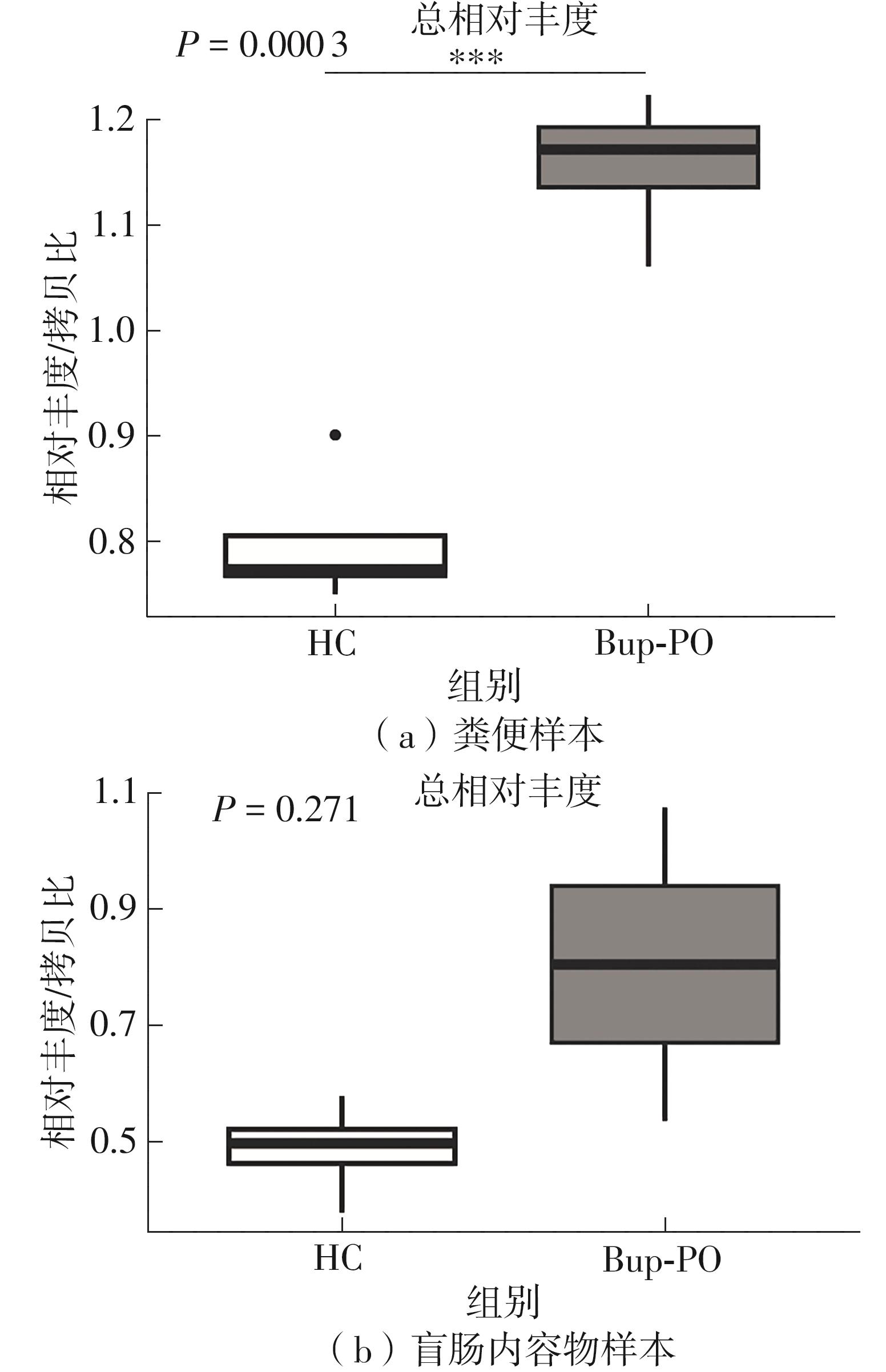
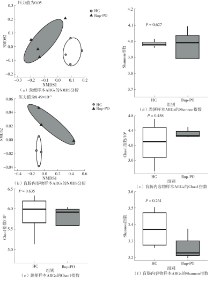
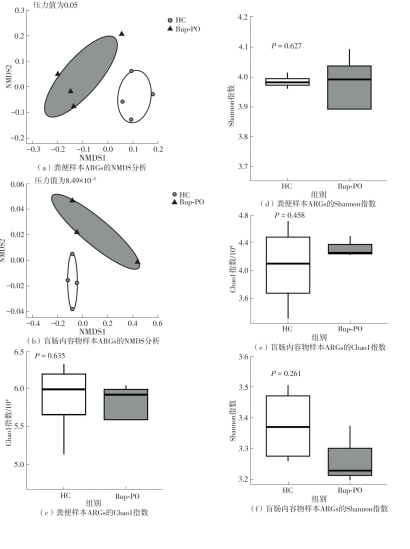
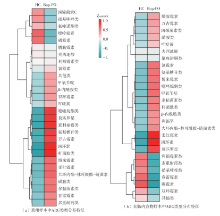
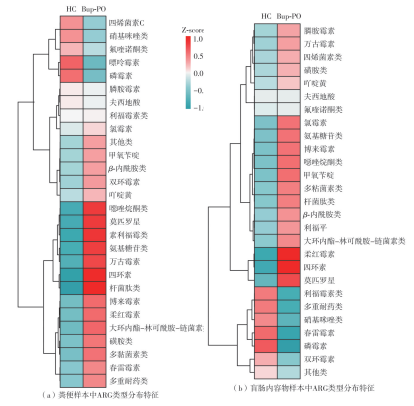
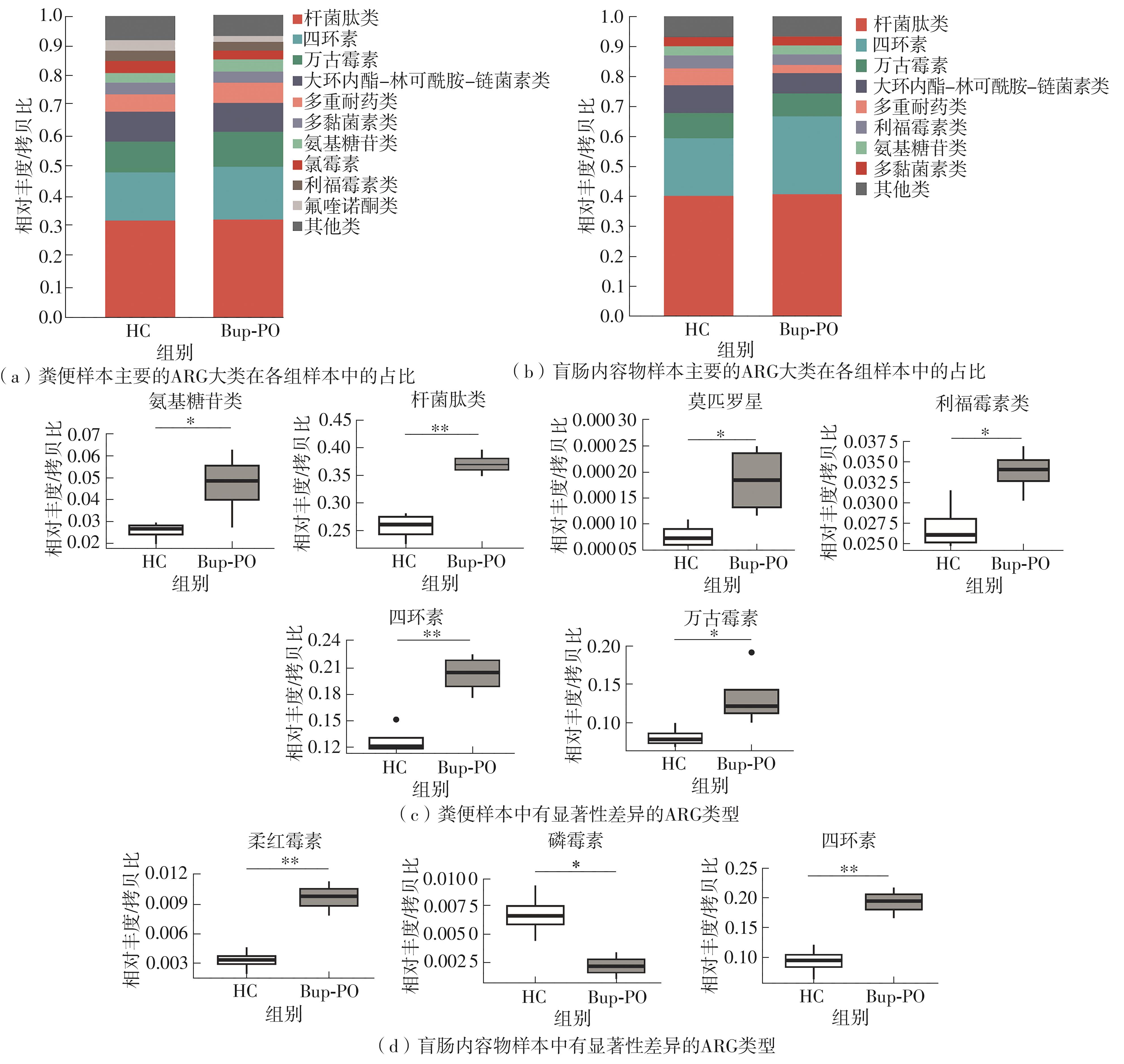
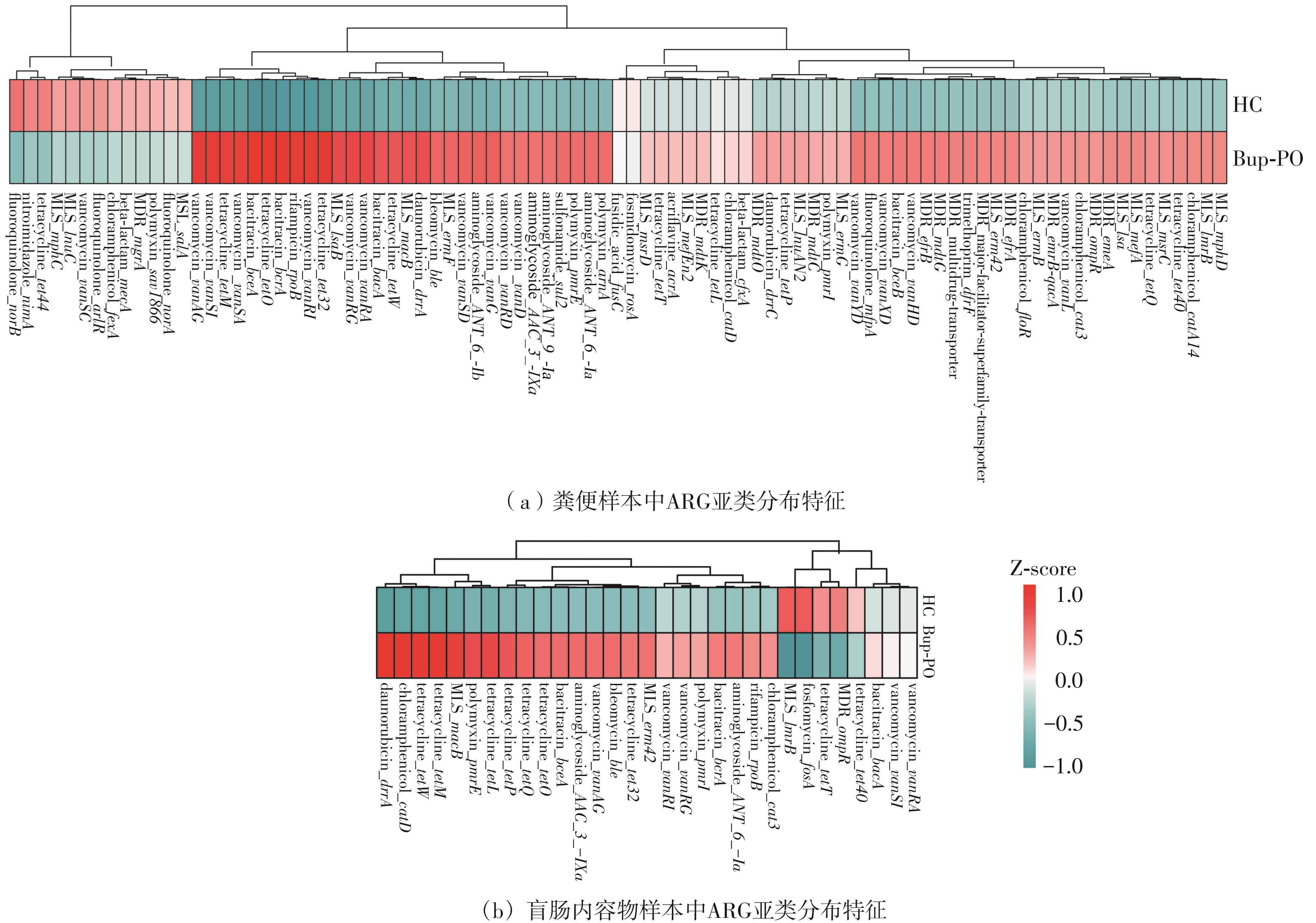
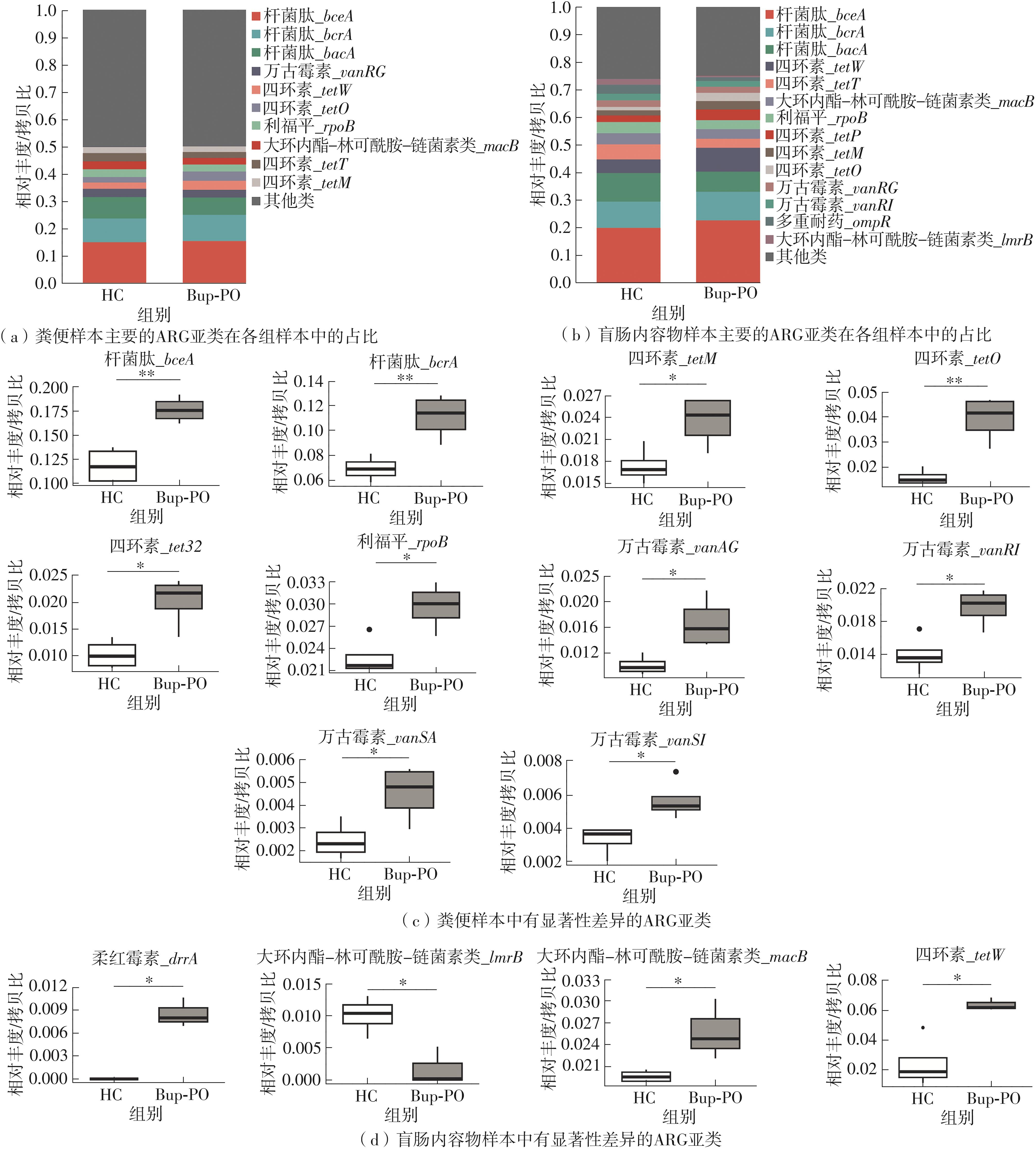
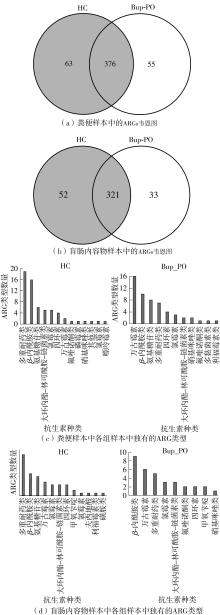
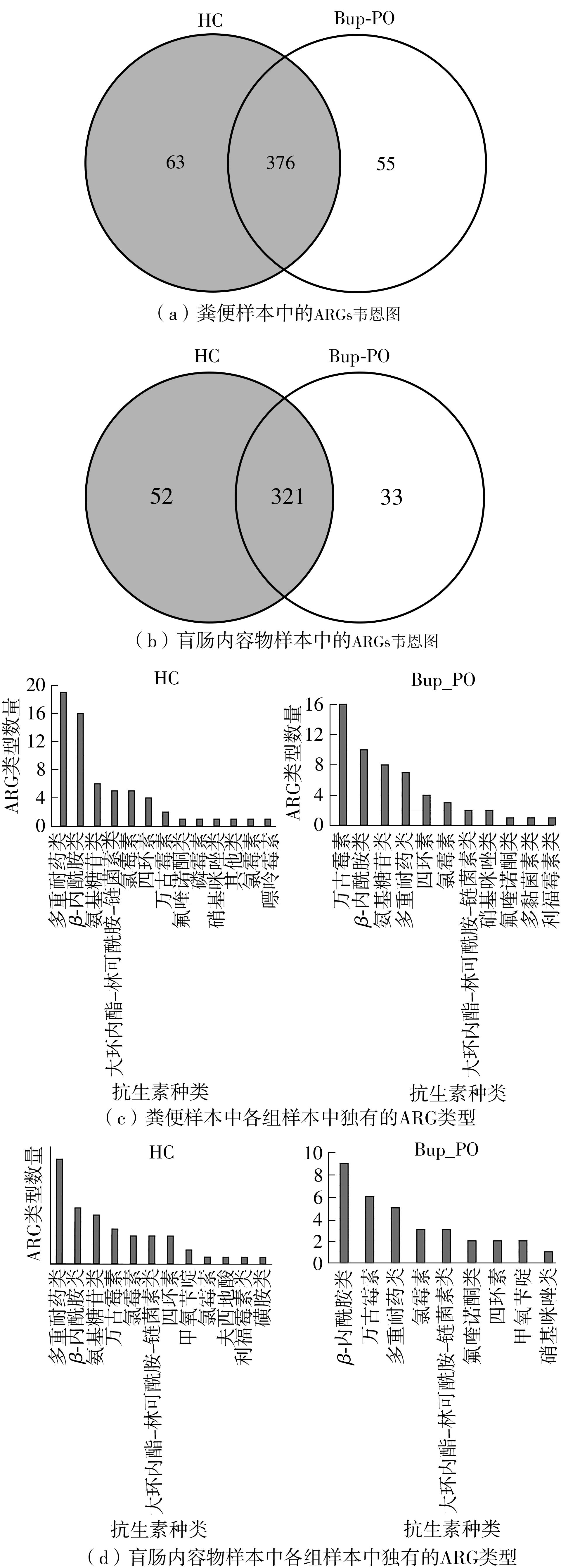
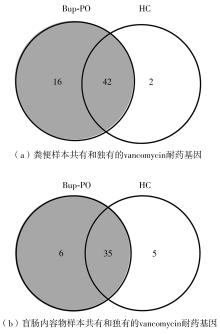
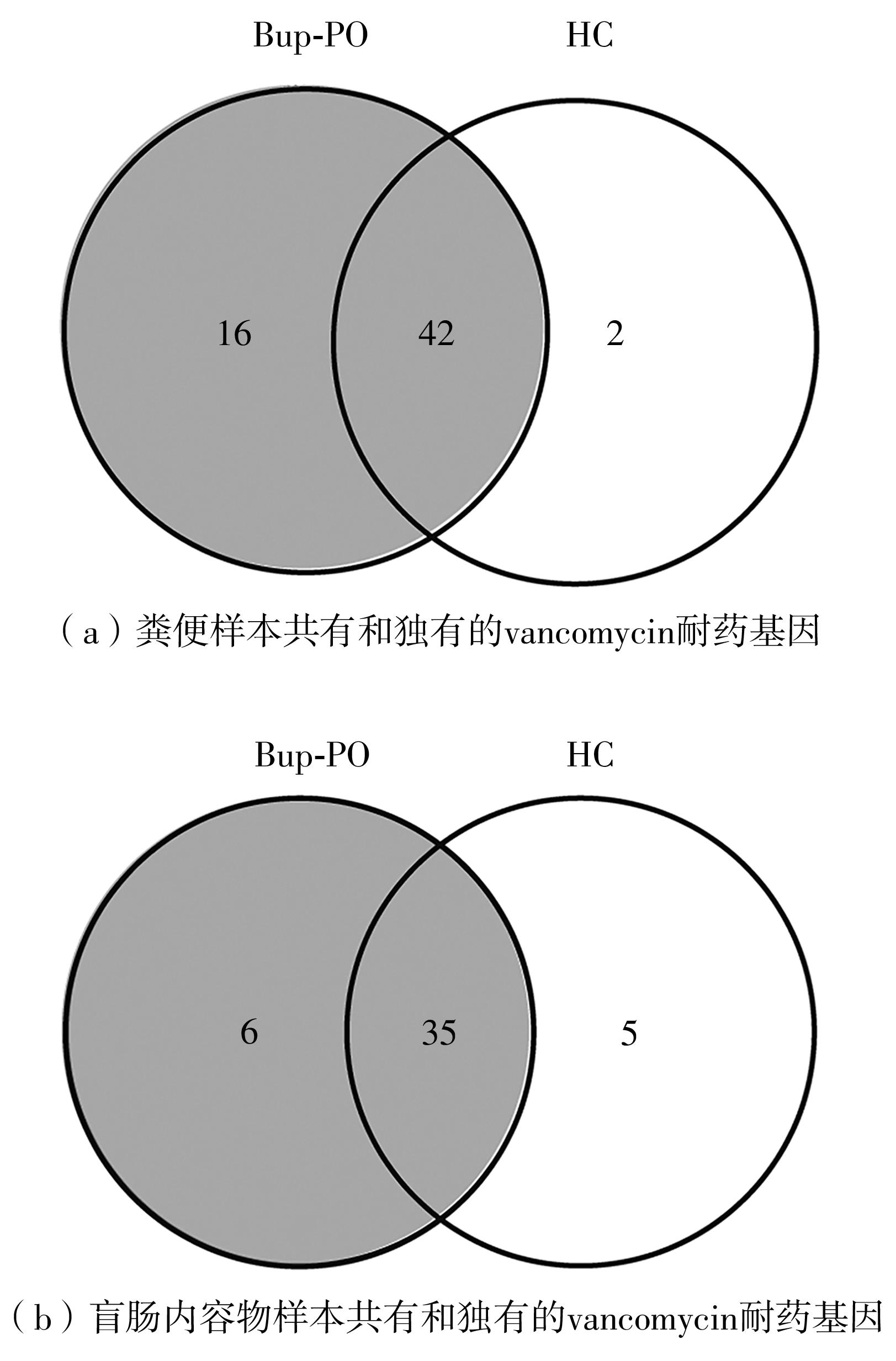
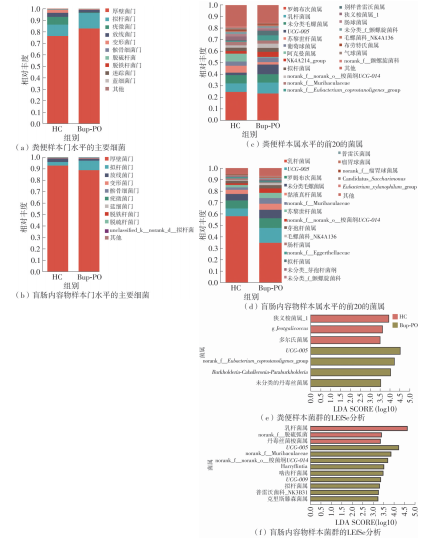
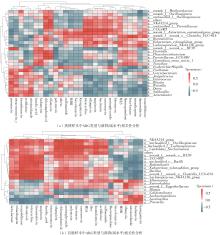
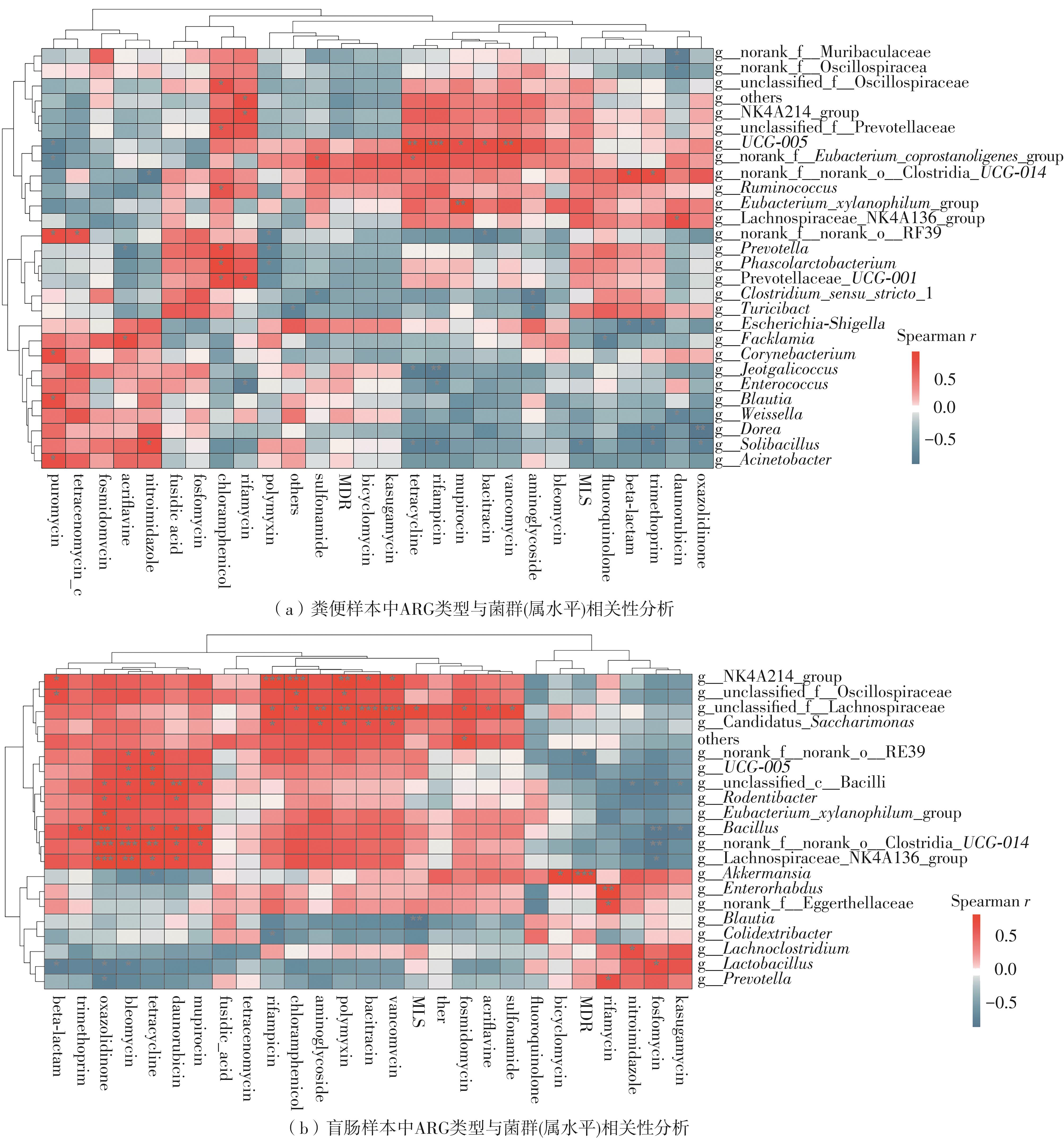
为探究抗抑郁药盐酸安非他酮对肠道菌群耐药组的影响,选用SD大鼠为研究对象,分别采用16S rRNA扩增子及宏基因组测序技术,分析盐酸安非他酮对大鼠粪便和盲肠内容物菌群及其耐药组的影响,并挖掘之间的关联。结果表明:粪便和盲肠内容物样本中主要抗生素耐药基因(ARGs)类型包括杆菌肽类、四环素、万古霉素及大环内酯-林可酰胺-链菌素类(MLS)等。与对照组(HC)相比,盐酸安非他酮灌胃干预组(Bup-PO)提高了大鼠粪便和盲肠内容物样本中细菌ARG总丰度,但仅在粪便样本中达到显著性差异。在ARG类型上,相比于HC组,Bup-PO组显著提高了粪便样本中氨基糖苷类、杆菌肽类、莫匹罗星、利福霉素类、四环素、万古霉素6类耐药基因类型的相对丰度,且增加了万古霉素抗性基因的种类。在盲肠内容物样本中,Bup-PO组显著提高了四环素、柔红霉素和磷霉素3类耐药基因类型的相对丰度。在ARG亚型上,在粪便样中,相比于HC组,Bup-PO组显著提高了万古霉素(vanAG、vanRI、vanSA、vanSI),四环素(tetM、tetO、tet32),杆菌肽类(bceA、bcrA)和利福霉素类( rpoB)耐药基因的相对丰度。在盲肠内容物样本中,灌胃盐酸安非他酮给药对ARGs的影响与粪便样本中有所不同,表现为降低了大环内酯-林可酰胺-链菌素类(lmrB)耐药基因的相对丰度,但提高了另一种大环内酯-林可酰胺-链菌素类(macB)耐药基因的相对丰度丰度。同时,灌胃给药盐酸安非他酮还提高了四环素(tetW)和柔红霉素(drrA)耐药基因的相对丰度。以上结果表明,盐酸安非他酮干预有增加大鼠肠道菌群抗生素耐药性的风险。UCG-005和norank_ f__norank_o__Clostridia_UCG-014是大鼠粪便和盲肠内容物菌群的主要细菌属,相关性分析结果表明,UCG-005可能是四环素、利福霉素类、莫匹罗星、杆菌肽类、万古霉素耐药基因的潜在细菌宿主,而norank_ f__norank_o__Clostridia_UCG-014可能是柔红霉素耐药基因的细菌宿主,它们在盐酸安非他酮给药后增加可能是导致这6种类型耐药基因丰度增加的原因。
中图分类号:
引用本文
闫鹤, 陈春霞, 刘宗保, 李佳林, 詹诗皿. 盐酸安非他酮对SD大鼠肠道菌群耐药组的影响[J]. 华南理工大学学报(自然科学版), 2025, 53(10): 155-173.
YAN He, CHEN Chunxia, LIU Zongbao, LI Jialin, ZHAN Shimin. Effects of Bupropion Hydrochloride on Resistome of Gut Microbiota in SD Rats[J]. Journal of South China University of Technology(Natural Science Edition), 2025, 53(10): 155-173.
| [1] | LAXMINARAYAN R, SRIDHAR D, BLASER M,et al .Achieving global targets for antimicrobial resistance[J/OL].Science,2016,353(6302):874-875. |
| [2] | 桑金慧,何振杰,余相宇,等 .基于宏基因组学分析安徽地区畜禽粪便微生物耐药性特征[J/OL].中国微生态学杂志,2024,36(1):29-40. |
| SANG Jinhui, HE Zhenjie, YU Xiangyu,et al .Macrogenomics-based analysis of microbial resistance of microbes in pig and chicken faeces in Anhui region[J].Chinese Journal of Microecology,2024,36(1):29-40. | |
| [3] | DING P, LU J, WANG Y,et al .Antidepressants promote the spread of antibiotic resistance via horizontally conjugative gene transfer[J/OL].Environmental Microbiology,2022,24(11):5261-5276. |
| [4] | MURRAY C J, IKUTA K S, SHARARA F,et al .Global burden of bacterial antimicrobial resistance in 2019:a systematic analysis[J/OL].Lancet,2022,399(10325):629-655. |
| [5] | GOOSSENS H, FERECH M, STICHELE R V,et al .Outpatient antibiotic use in Europe and association with resistance:a cross-national database study[J].Lancet,2005,365(9459):579-587. |
| [6] | LARSSON D G J, FLACH C F .Antibiotic resistance in the environment[J/OL].Nature Reviews.Microbiology,2022,20(5):257-269. |
| [7] | QIU Z, YU Y, CHEN Z,et al .Nanoalumina promotes the horizontal transfer of multiresistance genes mediated by plasmids across genera[J/OL].Proceedings of the National Academy of Sciences,2012,109(13):4944-4949. |
| [8] | WANG X, CHEN Z, MU Q,et al .Ionic liquid enriches the antibiotic resistome,especially efflux pump genes,before significantly affecting microbial community structure[J/OL].Environmental Science & Technology,2020,54(7):4305-4315. |
| [9] | WANG Y, LU J, MAO L,et al .Antiepileptic drug carbamazepine promotes horizontal transfer of plasmid-borne multi-antibiotic resistance genes within and across bacterial genera[J/OL].The ISME Journal,2019,13(2):509-522. |
| [10] | KIM S, COVINGTON A, PAMER E G .The intestinal microbiota:antibiotics,colonization resistance, and enteric pathogens[J/OL].Immunological Reviews,2017,279(1):90-105. |
| [11] | SCHMIDT H D, SHELTON R C, DUMAN R S .Functional biomarkers of depression:diagnosis,treatment,and pathophysiology[J/OL].Neuropsychopharmacology,2011,36(12):2375-2394. |
| [12] | FRIEDRICH M J .Depression is the leading cause of disability around the world[J/OL].The Journal of the American Medical Association,2017,317(15):1517. |
| [13] | 高鑫磊,贾艾楠,刘敏 .1990年和2019年中国分省精神障碍伤残负担分析[J].中华精神科杂志,2023,56(1):40-46. |
| GAO Xinlei, JIA Ainan, LIU Min,et al .The burden of disability associated with mental disorders in China by province between 1990 and 2019[J].Chinese Journal of Psychiatry,2023,56(1):40-46. | |
| [14] | DREW L .How antidepressants help bacteria resist antibiotics[J/OL].Nature,2023,doi:10.1038/d41586-023-00186-y . |
| [15] | CIPRIANI A, FURUKAWA T A, SALANTI G,et al .Comparative efficacy and acceptability of 21 antidepressant drugs for the acute treatment of adults with major depressive disorder:a systematic review and network meta-analysis[J/OL].Lancet,2018,391(10128):1357-1366. |
| [16] | WANG Y, YU Z, DING P,et al .Antidepressants can induce mutation and enhance persistence toward multiple antibiotics[J/OL].Proceedings of the National Academy of Sciences,2023,120(5):e2208344120/1-12. |
| [17] | ADU M K, WALLACE L J, LARTEY K F,et al .Prevalence and correlates of likely major depressive disorder among the adult population in ghana during the COVID-19 pandemic[J/OL].International Journal of Environmental Research and Public Health,2021,18(13):7106/1-19. |
| [18] | VERMA S, MISHRA A .Depression,anxiety,and stress and socio-demographic correlates among general Indian public during COVID-19[J/OL].International Journal of Social Psychiatry,2020,66(8):756-762. |
| [19] | SUNA S G, DIDEM K, ERYILMAZ M .The effects of antidepressants fluoxetine,sertraline,and amitriptyline on the development of antibiotic resistance in acinetobacter baumannii[J/OL].Archives of Microbiology,2022,204(4):230/1-10. |
| [20] | SHI D, HAO H, WEI Z,et al .Combined exposure to non-antibiotic pharmaceutics and antibiotics in the gut synergistically promote the development of multi-drug-resistance in Escherichia coli [J/OL].Gut Microbes,2022,14(1):2018901/1-17. |
| [21] | JIN M, LU J, CHEN Z,et al .Antidepressant fluoxetine induces multiple antibiotics resistance in Escherichia coli via ROS-mediated mutagenesis[J/OL].Environment International,2018,120:421-430. |
| [22] | OU J, ELIZALDE P, GUO H B,et al .TCA and SSRI antidepressants exert selection pressure for efflux-dependent antibiotic resistance mechanisms in Escherichia coli[J/OL].mBio,2022,13(6):e02191-22/1-20. |
| [23] | WANG Y, HU Y, CAO J,et al .Antibiotic resistance gene reservoir in live poultry markets[J/OL].The Journal of Infection,2019,78(6):445-453. |
| [24] | VICH VILA A, COLLIJ V, SANNA S,et al .Impact of commonly used drugs on the composition and metabolic function of the gut microbiota[J/OL].Nature Communications, 2020,11(1):362/1-11. |
| [25] | ZHANG W, QU W, WANG H,et al .Antidepressants fluoxetine and amitriptyline induce alterations in intestinal microbiota and gut microbiome function in rats exposed to chronic unpredictable mild stress[J/OL].Translational Psychiatry,2021,11(1):131/1-16. |
| [26] | ZUNG W W K, BRODIE H K H, FABRE L,et al .Comparative efficacy and safety of bupropion and placebo in the treatment of depression[J/OL].Psychopharmacology,1983,79(4):343-347. |
| [27] | JEFFERSON J W, PRADKO J F, MUIR K T .Bupropion for major depressive disorder:pharmacokinetic and formulation considerations[J].Clinical Therapeutics,2005,27(11):1685-1695. |
| [28] | JORENBY D E, HAYS J T, RIGOTTI N A,et al .Efficacy of varenicline,an α 4β2 nicotinic acetylcholine receptor partial agonist,vs placebo or sustained-release bupropion for smoking Cessation:a randomized controlled trial[J/OL].The Journal of the American Medical Association,2006,296(1):56-63. |
| [29] | FOLEY K F, DESANTY K P, KAST R E .Bupropion:pharmacology and therapeutic applications[J].Expert Review of Neurotherapeutics,2006,6(9):1249-1265. |
| [30] | VARSHOSAZ J, MINAIYAN M, ZAKI M R,et al .In vitro/in vivo evaluation of agar nano spheres for pulmonary delivery of bupropion HCl[J/OL].Drug Delivery,2016:23(6):1948-1954. |
| [31] | LAIZURE S C, DEVANE C L, STEWART J T,et al .Pharmacokinetics of bupropion and its major basic metabolites in normal subjects after a single dose[J/OL].Clinical Pharmacology and Therapeutics,1985,38(5):586-589. |
| [32] | STAHL S M, PRADKO J F, HAIGHT B R,et al .A review of the neuropharmacology of bupropion,a dual norepinephrine and dopamine reuptake inhibitor[J].Primary Care Companion to the Journal of Clinical Psychiatry,2004,6(4):159-166. |
| [33] | 周道友 .不同剂量盐酸安非他酮与帕罗西汀治疗抑郁症的临床对照研究[J].医学与哲学(临床决策论坛版),2009,30(9):34-35,51. |
| ZHOU Daoyou. Study of different dose of bupropion hydrochloride and paroxetine in treatment of depression[J].Medicine & Philosophy,2009,30(9):34-35,51. | |
| [34] | CARROLL F I, BLOUGH B E, MASCARELLA S W,et al .Bupropion and bupropion analogs as treatments for CNS disorders[M/OL].Advances in Pharmacology,2014,69:177-216. |
| [35] | BALLESTA A, ORIO L, ARCO R,et al .Bupropion,a possible antidepressant without negative effects on alcohol relapse[J/OL].European Neuropsychopharmacology,2019,29(6):756-765. |
| [36] | CHEN S, ZHOU Y, CHEN Y,et al .Fastp:an ultra-fast all-in-one FASTQ preprocessor[J/OL].Bioinformatics (Oxford,England),2018,34(17):i884-i890. |
| [37] | LI H, DURBIN R .Fast and accurate short read alignment with burrows-wheeler transform[J/OL].Bioinformatics (Oxford, England),2009,25(14):1754-1760. |
| [38] | BUCHFINK B, XIE C, HUSON D H .Fast and sensitive protein alignment using DIAMOND[J/OL].Nature Methods,2015,12(1):59-60. |
| [39] | LIU Z, KLÜMPER U, LIU Y,et al .Metagenomic and metatranscriptomic analyses reveal activity and hosts of antibiotic resistance genes in activated sludge[J/OL].Environment International,2019,129:208-220. |
| [40] | HU Y, YANG X, QIN J,et al .Metagenome-wide analysis of antibiotic resistance genes in a large cohort of human gut microbiota[J/OL].Nature Communications,2013,4(1):2151/1-7. |
| [41] | MA L, XIA Y, LI B,et al .Metagenomic assembly reveals hosts of antibiotic resistance genes and the shared resistome in pig, chicken, and human feces[J/OL].Environmental Science & Technology,2016,50(1):420-427. |
| [42] | YAO Y, LIU Z, YIP K K,et al .Cross-regional scale pollution of freshwater biofilms unveiled by antibiotic resistance genes[J/OL].Science of the Total Environment,2022,818(19):151835/1-12. |
| [43] | LI B, YANG Y, MA L,et al .Metagenomic and network analysis reveal wide distribution and co-occurrence of environmental antibiotic resistance genes[J/OL].The ISME Journal,2015,9(11):2490-2502. |
| [44] | CHEN B, YUAN K, CHEN X,et al .Metagenomic analysis revealing antibiotic resistance genes (ARGs) and their genetic compartments in the Tibetan environment[J/OL].Environmental Science & Technology,2016,50(13):6670-6679. |
| [45] | MACKELPRANG R, WALDROP M P, DEANGELIS K M,et al .Metagenomic analysis of a permafrost microbial community reveals a rapid response to thaw[J/OL].Nature,2011,480(7377):368-371. |
| [46] | MA L, LI B, ZHANG T .New insights into antibiotic resistome in drinking water and management perspectives:a metagenomic based study of small-sized microbes[J/OL].Water Research,2019,152:191-201. |
| [47] | QIU T, HUO L, GUO Y,et al .Metagenomic assembly reveals hosts and mobility of common antibiotic resistome in animal manure and commercial compost[J/OL].Environmental Microbiome,2022,17(1):42/1-15. |
| [48] | 钱璟,吴哲元,朱泳璋,等 .上海市崇明区猪-土壤界面微生态与抗生素耐药性相关性分析[J/OL].中国微生态学杂志,2024,36(2):135-146. |
| QIAN Jing, WU Zheyuan, ZHU Yongzhang,et al .Correlation between microecology and antibiotic resistance at the pig-soil interface in Chongming District,Shanghai,China[J/OL].Chinese Journal of Microecology,2024,36(2):135-146. | |
| [49] | FENG J, LI B, JIANG X,et al .Antibiotic resistome in a large-scale healthy human gut microbiota deciphered by metagenomic and network analyses[J/OL].Environmental Microbiology,2018,20(1):355-368. |
| [50] | BUNGAU S, TIT D M, BEHL T,et al .Aspects of excessive antibiotic consumption and environmental influences correlated with the occurrence of resistance to antimicrobial agents[J/OL].Current Opinion in Environmental Science & Health,2021,19:100224/1-6. |
| [51] | ZHANG R M, LIU X, WANG S L,et al .Distribution patterns of antibiotic resistance genes and their bacterial hosts in pig farm wastewater treatment systems and soil fertilized with pig manure[J/OL].Science of the Total Environment,2021,758:143654/1-7. |
| [52] | PAN X, QIANG Z,BEN W,et al .Residual veterinary antibiotics in swine manure from concentrated animal feeding operations in shandong province,China[J/OL].Chemosphere,2011,84(5):695-700. |
| [53] | SHENG S, LI X, ZHAO S,et al .Effects of levodopa on gut bacterial antibiotic resistance in Parkinson's disease rat[J/OL].Frontiers in Aging Neuroscience,2023, 15:1122712/1-12. |
| [54] | AMMAM F, MEZIANE-CHERIF D, MENGIN-LECREULX D,et al .The functional vanGCd cluster of clostridium difficile does not confer vancomycin resistance[J/OL].Molecular Microbiology,2013,89(4):612-625. |
| [55] | ARIAS C, COURVALIN P, REYNOLDS P . vanC cluster of vancomycin-resistant Enterococcus gallinarum BM4174[J/OL].Antimicrobial Agents and Chemotherapy,2000,44(6):1660-1666. |
| [56] | COURVALIN P .Vancomycin resistance in gram-positive cocci[J/OL].Clinical Infectious Diseases: An Official Publication of the Infectious Diseases Society of America,2006,42 ():S25-S34. |
| [57] | KAPLAN E L .Vancomycin in infants and children: a review of pharmacology and indications for therapy and prophylaxis[J/OL].Journal of Antimicrobial Chemotherapy,1984,14():59-66. |
| [58] | WILHELM M P .Vancomycin[J/OL].Mayo Clinic Proceedings,1991,66(11):1165-1170. |
| [59] | ARIAS C A, MURRAY B E .The rise of the Enterococcus:beyond vancomycin resistance[J/OL].Nature Reviews.Microbiology,2012,10(4):266-278. |
| [60] | STANLEY D, GEIER M S, CHEN H,et al .Comparison of fecal and cecal microbiotas reveals qualitative similarities but quantitative differences[J/OL].BMC Microbiology,2015,15:51. |
| [61] | CHE Y, XIA Y, LIU L,et al .Mobile antibiotic resistome in wastewater treatment plants revealed by Nanopore metagenomic sequencing[J/OL].Microbiome,2019,7(1):44. |
| [62] | HE L Y, HE L K, LIU Y S,et al .Microbial diversity and antibiotic resistome in swine farm environments[J/OL].Science of the Total Environment,2019,685:197-207. |
| [63] | WEI B, XU Q L, ZHANG B,et al .Comparative study of Sargassum fusiforme polysaccharides in regulating cecal and fecal microbiota of high-fat diet-fed mice[J/OL].Marine Drugs,2021,19(7):364/1-11. |
| [64] | TANCA A, MANGHINA V, FRAUMENE C,et al .Metaproteogenomics reveals taxonomic and functional changes between cecal and fecal microbiota in mouse[J/OL].Frontiers in Microbiology,2017,8:391/1-12. |
| [65] | SUN C H, LIU H Y, LIU B,et al .Analysis of the gut microbiome of wild and captive Père david's deer[J/OL].Frontiers in Microbiology,2019,10:2331/1-9. |
| [66] | HAWORTH S E, WHITE K S, CÔTÉ S D,et al .Space,time and captivity: quantifying the factors influencing the fecal microbiome of an alpine ungulate[J/OL].FEMS Microbiology Ecology,2019,95(7):fiz095. |
| [67] | LI J G, WANG C D, TANG Z H,et al .The gut bacterial community composition of wild Cervus albirostris (white-lipped deer) detected by the 16S ribosomal RNA gene sequencing[J/OL].Current Microbiology,2017,74(9):1100-1107. |
| [68] | COUCH C E, STAGAMAN K, SPAAN R S,et al .Diet and gut microbiome enterotype are associated at the population level in african buffalo[J/OL].Nature Communications,2021,12(1):2267/1-11. |
| [69] | SUN G, ZHANG H, WEI Q,et al .Comparative analyses of fecal microbiota in European mouflon (Ovis orientalis musimon) and blue sheep (Pseudois nayaur) living at low or high altitudes[J/OL].Frontiers in Microbiology,2019,10:1735/1-15. |
| [70] | LI Y, YAN Y, FU H,et al .Does diet or macronutrients intake drive the structure and function of gut microbiota?[J/OL].Frontiers in Microbiology,2023,14:1126189/1-13. |
| [71] | ZHANG B, WAN Y, ZHOU X,et al .Characteristics of serum metabolites and gut microbiota in diabetic kidney disease[J/OL].Frontiers in Pharmacology,2022,13:872988/1-17. |
| [72] | WANG D, ZHOU Y, ZHAO J,et al .Oral yak whey protein can alleviate UV-induced skin photoaging and modulate gut microbiota composition[J/OL].Foods,2024,13(16):2621/1-14. |
| [73] | RAINERI S, SHERRIFF J A, THOMPSON K S J,et al .Pharmacologically induced weight loss is associated with distinct gut microbiome changes in obese rats[J/OL].BMC Microbiology,2022,22(1):91/1-21. |
| [74] | SONG E J, SHIN N R, JEON S,et al .Impact of the herbal medicine,Ephedra sinica stapf,on gut microbiota and body weight in a diet-induced obesity model[J/OL].Frontiers in Pharmacology,2022,13:1042833/1-11. |
| [1] | 韩源平, 徐思雅, 蒋希乐. 补充维生素D对非酒精性脂肪肝病患者肠道菌群的影响[J]. 华南理工大学学报(自然科学版), 2022, 50(11): 62-73. |
| [2] | 张智, 包智影, 孙家佳, 等. 发酵黄精多糖对肥胖小鼠肠道菌群的影响[J]. 华南理工大学学报(自然科学版), 2021, 49(3): 95-105,113. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||